If you've ever been sent for a heart exam after feeling chest pressure, you likely faced two choices: a standard electrocardiogram or a stress test. Both look at your heart's electrical system, but they catch different problems. In fact, doctors perform over 11 million stress tests every year in the United States alone. Why? Because a quiet heart often hides trouble until it hits hard.
Electrocardiogram, commonly known as an ECG or EKG, is a non-invasive procedure that records the heart's electrical activity using electrodes placed on the skin. Think of it as a snapshot of your heart's rhythm at rest. Developed by Willem Einthoven back in 1903, this tool remains the foundation of modern heart care. Today, however, many patients require more than a static image. This is where the stress test becomes essential.
The Difference Between Resting and Stressed Hearts
A resting ECG captures exactly what happens when you sit still. It can spot arrhythmias or signs of a past heart attack immediately. But imagine trying to diagnose a car engine while it's idling in the driveway. You might miss a sputter that only appears when you push the pedal to the floor. That is the exact limitation of a standard resting trace.
Stress Test is a diagnostic procedure that evaluates heart function during physical exertion or pharmacological stimulation. By increasing demand on the heart muscle, we force blood flow through narrowed arteries. If a vessel is blocked, the heart struggles to get oxygen during this high-demand state, showing changes the machine can read.
Clinicians generally recommend stress testing for patients with intermediate risk for Coronary Artery Disease. Guidelines from the American College of Cardiology suggest this approach works best when there is a 15% to 65% likelihood of blockage. For low-risk patients, the test adds cost without changing the outcome much. For high-risk patients, more direct imaging like angiography is usually next. The sweet spot lies in those confusing middle cases where chest pain exists, but nothing shows up on a paper EKG.
Types of Stress Testing Available Today
Not all stress tests involve running on a treadmill. Depending on your physical ability and specific symptoms, doctors choose between several variations. Understanding the options helps reduce anxiety before the appointment.
| Test Type | Primary Use | Radiation Exposure | Sensitivity Rate |
|---|---|---|---|
| Exercise Stress Test | Evaluates functional capacity and ECG changes during movement | None | 68% |
| Stress Echocardiogram | Uses ultrasound imaging to view heart walls moving under strain | None | 82% |
| Nuclear Stress Test | Tracks blood flow using radioactive tracers to detect perfusion defects | Moderate (9-12 mSv) | 85% |
| Chemical Stress Test | Used when patients cannot walk or run due to mobility issues | Varies by method | High accuracy |
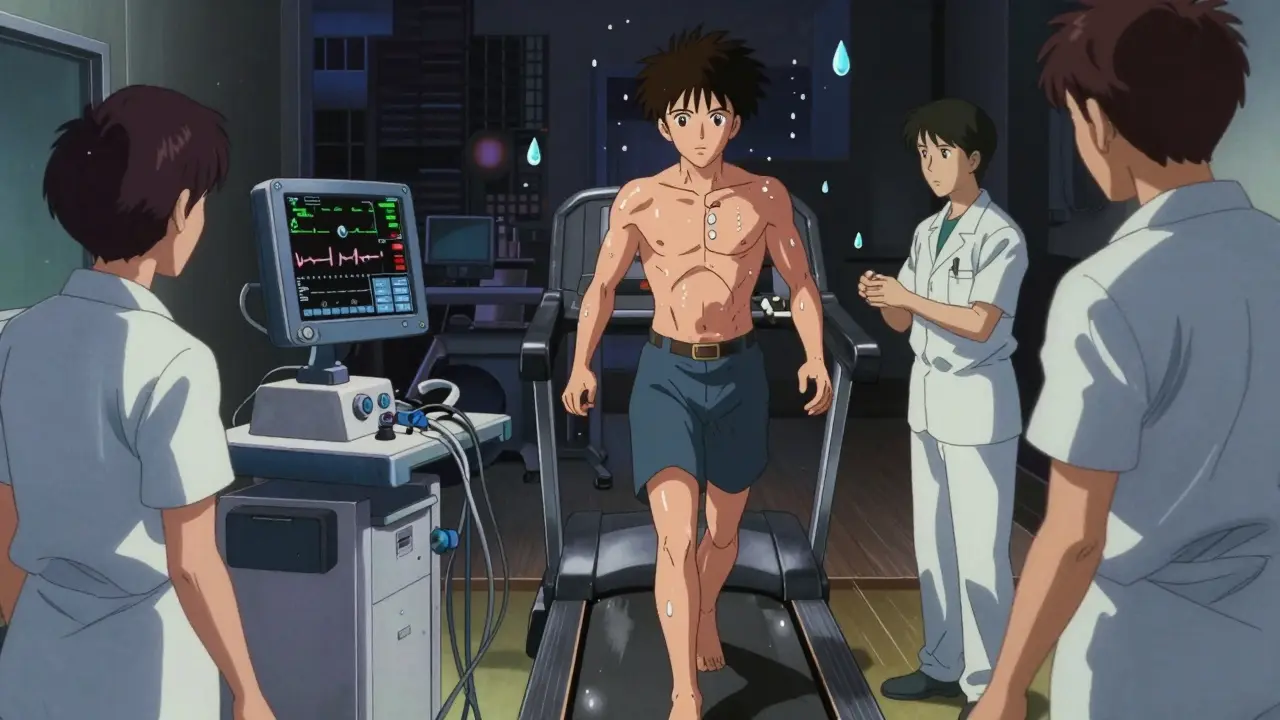
The most common protocol used globally is the Bruce Protocol. It starts the treadmill at 1.7 miles per hour with a steep incline and ramps up speed and elevation every three minutes. The goal is to reach 85% of your maximum predicted heart rate. This target is calculated by subtracting your age from 220. Reaching this milestone confirms your cardiovascular fitness level.
If you cannot walk, perhaps due to knee surgery or arthritis, doctors use medication to mimic the effect of exercise. Agents like adenosine or dipyridamile relax blood vessels in healthy hearts while blocked vessels remain tight. This creates a contrast visible on imaging. While effective, these chemicals can cause flushing or shortness of breath, which often scares patients. Remember, these sensations last only minutes and pass quickly once the infusion stops.
Preparing for Your Appointment
Success depends heavily on what you do before walking into the clinic. The preparation phase is simple but strict. Most importantly, avoid caffeine for 24 hours prior to testing. Coffee, energy drinks, and even dark chocolate interfere with the way your heart responds to stress. These stimulants can mask the warning signs the doctor is looking for.
You should wear comfortable clothing. A t-shirt that allows easy placement of sticky electrodes on your chest is ideal. Women may need a tank top to avoid removing undergarments unnecessarily. Eating a heavy meal right before the test is discouraged because digestion diverts blood flow away from muscles and heart, potentially causing nausea during the exertion.
Bring a list of medications you take regularly. Some drugs slow heart rate, such as beta-blockers. Your doctor might ask you to pause these days before testing to get a true measure of your heart's capability. Never stop medication without explicit instruction, though. Always confirm the dosage timing with the scheduling nurse.
What Happens During the Procedure
Once you arrive, a technician will attach sensors. An exercise session typically lasts 10 to 15 minutes total. A chemical stress test takes longer, roughly 30 to 60 minutes including setup. Throughout the process, four metrics stay under surveillance:
- Heart Rate: Monitored via continuous ECG leads.
- Blood Pressure: Checked every few minutes by manual cuff.
- Respiratory Function: Oxygen saturation measured constantly.
- Electrical Signals: Watching for ST-segment changes on the graph.
It feels like working out at the gym, except you are surrounded by medical staff ready to help. If you feel dizzy or have severe pain, you tell them immediately. They can stop the machine instantly. Most people finish the full protocol, but stopping early due to safety limits is also a valid result.
Interpreting the Data
Afterward, a cardiologist reviews the waveforms. They aren't just looking at lines; they are hunting for ischemia, which means insufficient blood flow. One classic sign is ST-segment depression. If the line dips significantly during peak effort, it suggests oxygen starvation. Another key indicator is functional capacity. Each additional minute you spend exercising correlates with a lower risk of future heart events. Studies show an extra minute of endurance equals about a 12% drop in cardiac risk.
However, no test is perfect. A standard ECG stress test has about 68% sensitivity for finding blockages. This means false negatives happen, especially in women with microvascular dysfunction. Newer technology aims to fix this. Artificial intelligence algorithms introduced recently can improve interpretation accuracy by over 18%. Machine learning reads patterns in the data that human eyes often miss.
Results also vary by facility quality. Academic centers often provide comprehensive reports averaging over 3 pages, while smaller clinics might stick to a summary. Ask for the detailed report if you plan to see another specialist later. Clear documentation prevents repeat testing down the road.
Looking Ahead: Technology and Safety
Cardiovascular diagnostics are evolving rapidly. Portable devices like the FDA-cleared Cardiac Dynamics StressPal now allow testing outside traditional hospitals with high agreement rates compared to big treadmills. Meanwhile, safety protocols have tightened regarding radiation. Nuclear tests, while highly sensitive, expose patients to background radiation equivalent to several years of natural exposure. Facilities now use low-dose optimization to cut this exposure by 35% since 2021.
We must acknowledge limitations too. Dr. Emily Chen notes that premenopausal women often face higher false-negative rates due to physiological differences in how their coronary microcirculation functions. If you fit this group and have persistent symptoms despite normal stress tests, your doctor might order a CT angiogram instead to bypass these biological variables.
The future points toward hybrid methods. Combining stress echo with speckle-tracking strain analysis improves detection of subtle weaknesses from 68% to 89% in specific populations. As technology matures, the goal is to keep testing non-invasive while catching more silent dangers before they turn into emergencies.
Is a stress test painful?
Most people do not experience pain. Physical fatigue is common, similar to a workout. Chemical stress agents can cause brief flushing or warmth, but discomfort is temporary.
How long does the test take?
A standard exercise test takes 10 to 15 minutes of actual walking. Chemical tests are longer, often 30 to 60 minutes including monitoring.
Can I eat before the test?
Avoid heavy meals beforehand. Light eating is okay, but skip caffeine entirely for 24 hours to prevent skewed results.
Who performs the test?
Certified technicians set up the equipment, but a physician or experienced provider monitors the vital signs throughout the session.
Are there risks involved?
Serious risks are rare. Common side effects include mild dizziness or temporary chest discomfort. Doctors avoid testing unstable patients to ensure safety.

Sabrina Herciu
You absolutely MUST avoid coffee beforehand! It interferes significantly with adenosine receptors!! Many patients forget this vital step!!! The results become unreliable immediately... Do not risk getting a bad result!! That is dangerous!!!! Stick to water only! Hydration is key!!
Philip Wynkoop
good info thanks :)
Debra Brigman
Listening to your own body requires immense patience in modern times. Machines interpret complex biological data with limited precision. We place blind faith in technology without questioning its limits. A solitary heartbeat tells a profound narrative of survival. Each distinct rhythm holds a hidden secret from the past. Doctors read the jagged lines on printed paper constantly. They frequently miss the living soul behind the electrical signal. Stress testing forces the physiological truth out under pressure. It successfully mimics the daily chaos of human existence. Physical exercise reveals hidden weaknesses in the coronary arteries. Complete rest often hides many potentially dangerous issues. Excessive caffeine clouds the objective judgment of diagnostic tools. Thorough preparation dramatically changes the entire clinical outcome. Ignoring simple prep routines ruins the precious diagnostic window completely. We must respect the rigorous science involved in every test. Understanding the nuance saves lives in the long run.
gina macabuhay
The implication that caffeine ruins diagnostics is hyperbolic. Most patients drink tea regardless of protocols. Compliance rates remain abysmally low in general populations. Your suggestion ignores real-world patient behavior patterns entirely. People prioritize convenience over medical accuracy frequently.
Monique Louise Hill
Oh my goodness! You need to listen to medical professionals! They know best! 😊 Don’t take risks with your health! ❤️ Listen to the doctor! 🛑 Coffee is bad! 🚫 Stay safe always! 💖
Aaron Olney
I had a felling of death last year! My chest hurt real bad. The treamill broke down mid way. Docotor said i was fine but i knew! It scares me now to walk even. U feel alone when ur healt gets tested. Why do they rush us? Its scary being hooked up!
Jordan Marx
From a functional capacity perspective, reaching 85 percent max predicted heart rate is critical for accurate stratification. The Bruce protocol ensures adequate metabolic demand during the ischemic threshold evaluation. Clinicians must monitor ST-segment depression dynamically throughout the exertion phase. Perfusion defects visible on nuclear imaging correlate strongly with significant stenosis. Optimizing medication timing prior to testing reduces beta-blockade interference effectively. Remember that pharmacological agents induce vasodilation similar to exercise states. Safety margins remain paramount when utilizing high-intensity treadmill slopes. Always validate findings against baseline resting ECG parameters. Interpretation requires integrating hemodynamic response data with symptom reporting. Comprehensive risk assessment benefits greatly from standardized stress methodology application.
Sophie Hallam
That sounds like excellent advice for anyone preparing. It is good to understand the mechanics before going in. Knowing what to expect helps reduce anxiety levels significantly. Thank you for sharing the technical details clearly. It makes the process seem much less frightening. Everyone deserves to feel prepared for their appointment.